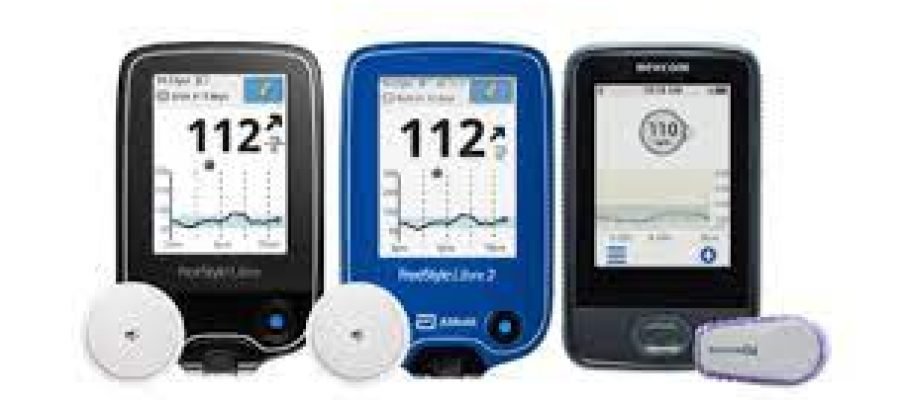
Continuous glucose monitors (CGMs) are wearable diabetes tools that monitor and alarm for changes in your glucose. CGMs are different from glucometers (glucose meters) because they can only tell you what your glucose is, right now.
There are three parts to a CGM system: A self-inserted sensor that sits under the skin for up to 14 days, a transmitter that sends glucose information, and a receiver for glucose data (a smartphone, insulin pump, or other hand-held devices).
While both can tell you what your real-time glucose is, CGMs help to detect patterns over time. This is because they provide glucose numbers every few minutes. Everyone’s diabetes is different. Your provider will suggest what’s best for you and your diabetes management.
Become a “diabetes detective”
In order to make effective changes in your diabetes care, you’ll need to become a “diabetes detective.” Here’s how:
- Know your numbers: Use a glucometer or a CGM
- Understand what your target range is — if you’re unsure, ask your diabetes care team
- Keep an eye out for patterns
- Look for common reasons that may be affecting your glucose: Exercise, medications, food, illness, and stress are some examples
- Talk to your care team about your findings
- Make adjustments with their guidance
Improving your time in range starts by identifying your numbers and making small adjustments in response to them. You’ll begin to feel more comfortable over time making these changes on your own.
What are normal glucose levels?
The ADA glucose targets for non-pregnant adults are as follows. Your diabetes care team may have modifications from these numbers. Be sure to follow your diabetes care plan and personalized targets.
In general, glucose target ranges are:
- 80 mg/dl to 130 mg/dl before meals
- 180 mg/dl or lower two hours after starting a meal
- A1C less than 7%
Why is alerting important?
Alerting is important for awareness. CGMs can predict where your glucose is going, so you can take corrective steps before there’s a problem. This can be important, especially during physical activity and overnight when you’re sleeping. You can also choose to share your CGM data with another person, so they can receive alerts, too.
By monitoring trends over time, you can begin to see patterns and make adjustments to flatten glucose variability. This can help you to reach your glucose targets sooner. While blood glucose will always be changing, you can take steps to decrease the ups and downs.
What are CGM options?
There are a variety of CGM systems. The American Diabetes Association (ADA) has done the hard work of sifting through their differences. Check out the ADA Consumer Guide to compare the differences between the brands. You’ll need a prescription, and your insurance plan may prefer one over another. If you’re interested in CGM, ask your diabetes care team for more details.
How expensive is CGM monitoring?
Pricing varies from system to system. It’s important to know what your out-of-pocket costs will be. While Medicare supplies coverage for people with diabetes, you’ll have to meet certain criteria. Whether you have Medicare or private insurance, reach out and talk to customer service and learn more about CGM coverage.
Talk to someone specially trained to understand what people with Diabetes need to manage their Diabetes on a daily basis, Click Here.
Please review our business at: Google Yelp Facebook
If you’d like to learn more, please visit our Member’s Area to access our subscribed content.
Did you know you can work out and exercise with a trainer at your home, office, hotel room, or pretty much anywhere in the world with online personal training?
Like us on Facebook/Connect with us on LinkedIn/Follow us on Twitter
Make sure to forward this to friends and followers!